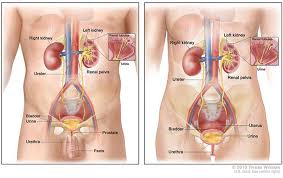
Kidney cancer
The kidneys are two bean-shaped organs, each about the size of a fist and they lie in our abdomen on each side of the spine. Their main job is to clean or filter the blood and make urine.
In some cases, kidney cells grow out of control, forming a tumour/cancer. Cancers caught early are easier to treat successfully. However, these tumours can grow to be quite large before they are detected.
Certain factors appear to increase the risk of getting kidney cancer like:
- Smoking
- Male sex
- Obesity
- Certain drugs
- Long-term dialysis
- Genetic conditions, such as von Hippel-Lindau (VHL) disease or inherited papillary renal cell carcinoma
- Having a family history of kidney cancer. The risk is especially high in siblings.
- Being exposed to certain chemicals, such as asbestos, cadmium, benzene, organic solvents, or certain herbicides
- Having high blood pressure. Doctors don’t know whether high blood pressure or medication used to treat it is the source of the increased risk.
Symptoms of Kidney Cancer:
Person may have one or more of these kidney cancer symptoms:
- Blood in your urine
- A lump in your side or abdomen
- A loss of appetite
- A pain in your side that doesn’t go away
- Weight loss that occurs for no known reason
- Fever that lasts for weeks and isn’t caused by a cold or other infection
- Extreme fatigue
Diagnosis:
Doctor will also order one or more tests like these:
- Urine tests check for blood in your urine or other signs of problems.
- Blood tests show how well your kidneys are working.
- Ultrasound may show a mass in the kidney
- A CT Scan. This may also require an injection of dye. CT scans have virtually replaced pyelogram and ultrasound as a tool for diagnosing kidney cancer.
- Magnetic Resonance Imaging
Treatment:
Surgery for removal of kidney along with its adjacent fascia (Radical Nephrectomy) may be a cure in early stages. In late stages other treatment modalities like special drugs may be required.
Bladder cancer
Bladder cancer is a common type of cancer that begins in the cells of the Urinary bladder.
Bladder cancer most often begins in the cells (urothelial cells) that line the inside of your bladder. Urothelial cells are also found in your kidneys and the tubes (ureters) that connect the kidneys to the bladder. Urothelial cancer can happen in the kidneys and ureters, too, but it’s much more common in the bladder.
Most bladder cancers are diagnosed at an early stage, when the cancer is highly treatable. But even early-stage bladder cancers can come back after successful treatment. For this reason, people with bladder cancer typically need follow-up tests for years after treatment to look for bladder cancer that recurs.
Symptoms
Bladder cancer signs and symptoms may include:
- Blood in urine (hematuria), which may cause urine to appear bright red or cola colored, though sometimes the urine appears normal and blood is detected on a lab test
- Frequent urination
- Painful urination
- Back pain
Risk factors
Factors that may increase bladder cancer risk include:
- Smoking can increase your risk of cancer.
- Increasing age. Bladder cancer risk increases as you age. Though it can occur at any age, most people diagnosed with bladder cancer are older than 55.
- Being male. Men are more likely to develop bladder cancer than women are.
- Exposure to certain chemicals. Your kidneys play a key role in filtering harmful chemicals from your bloodstream and moving them into your bladder. Because of this, it’s thought that being around certain chemicals may increase the risk of bladder cancer. Chemicals linked to bladder cancer risk include arsenic and chemicals used in the manufacture of dyes, rubber, leather, textiles and paint products.
- Previous cancer treatment. Treatment with the anti-cancer drug cyclophosphamide increases the risk of bladder cancer. People who received radiation treatments aimed at the pelvis for a previous cancer have a higher risk of developing bladder cancer.
- Chronic bladder inflammation. Chronic or repeated urinary infections or inflammations (cystitis), such as might happen with long-term use of a urinary catheter, may increase the risk of a squamous cell bladder cancer. In some areas of the world, squamous cell carcinoma is linked to chronic bladder inflammation caused by the parasitic infection known as schistosomiasis.
- Personal or family history of cancer. If you’ve had bladder cancer, you’re more likely to get it again. If one of your blood relatives — a parent, sibling or child — has a history of bladder cancer, you may have an increased risk of the disease, although it’s rare for bladder cancer to run in families. A family history of Lynch syndrome, also known as hereditary nonpolyposis colorectal cancer (HNPCC), can increase the risk of cancer in the urinary system, as well as in the colon, uterus, ovaries and other organs
Tests and procedures used to diagnose bladder cancer may include:
- Using a scope to examine the inside of your bladder (cystoscopy). To perform cystoscopy, your doctor inserts a small, narrow tube (cystoscope) through your urethra. The cystoscope has a lens that allows your doctor to see the inside of your urethra and bladder, to examine these structures for signs of disease. Cystoscopy can be done in a doctor’s office or in the hospital.
- Removing a sample of tissue for testing (biopsy). During cystoscopy, your doctor may pass a special tool through the scope and into your bladder to collect a cell sample (biopsy) for testing. This procedure is sometimes called transurethral resection of bladder tumor (TURBT). TURBT can also be used to treat bladder cancer.
- Examining a urine sample (urine cytology). A sample of your urine is analyzed under a microscope to check for cancer cells in a procedure called urine cytology.
- Imaging tests. Imaging tests, such as computerized tomography (CT) urogram or retrograde pyelogram, allow your doctor to examine the structures of your urinary tract.
During a CT urogram, a contrast dye injected into a vein in your hand eventually flows into your kidneys, ureters and bladder. X-ray images taken during the test provide a detailed view of your urinary tract and help your doctor identify any areas that might be cancer.
Retrograde pyelogram is an X-ray exam used to get a detailed look at the upper urinary tract. During this test, your doctor threads a thin tube (catheter) through your urethra and into your bladder to inject contrast dye into your ureters. The dye then flows into your kidneys while X-ray images are captured.
Determining the extent of the cancer
After confirming that you have bladder cancer, your doctor may recommend additional tests to determine whether your cancer has spread to your lymph nodes or to other areas of your body.
Tests may include:
- CT scan
- Magnetic resonance imaging (MRI)
- Positron emission tomography (PET)
- Bone scan
- Chest X-ray
Treatment
Treatment options for bladder cancer depend on a number of factors, including the type of cancer, grade of the cancer and stage of the cancer, which are taken into consideration along with your overall health and your treatment preferences.
Bladder cancer treatment may include:
- Surgery, to remove the cancer cells
- Chemotherapy in the bladder (intravesical chemotherapy), to treat cancers that are confined to the lining of the bladder but have a high risk of recurrence or progression to a higher stage
- Chemotherapy for the whole body (systemic chemotherapy), to increase the chance for a cure in a person having surgery to remove the bladder, or as a primary treatment when surgery isn’t an option
- Radiation therapy, to destroy cancer cells, often as a primary treatment when surgery isn’t an option or isn’t desired
- Immunotherapy, to trigger the body’s immune system to fight cancer cells, either in the bladder or throughout the body
- Targeted therapy, to treat advanced cancer when other treatments haven’t helped
A combination of treatment approaches may be recommended by your doctor and members of your care team.
Prostate Cancer
Cancer that starts in the prostate (the gland under a man’s bladder that produces seminal fluid) is called prostate cancer. Prostate cancer is the most common type of cancer among men, not including skin cancer.
Risks
There is no known cause for prostate cancer, but there are certain factors that can increase a man’s risk of getting prostate cancer, including:
- Age: The risk of getting prostate cancer increases with age.
- Ethnicity: African-American men are more likely to get the disease and they are more likely to have more aggressive tumors.
- Family History: Men who have a history of prostate cancer in the family are more likely to get it themselves.
- Testosterone Levels: Higher levels of testosterone are associated with increased rate of prostate cancer growth and spread. This is why men on testosterone replacement must have prostate cancer screening every 6 months.
- Smoking: Some studies have shown that the risk of developing cancer of the prostate can double in heavy smokers. Quitting can bring your risk down.
- Lifestyle and Location: Diet and lifestyle may increase the risk of developing the disease. Also, people in North America and Northern Europe have higher incidences of the disease.
Symptoms
Most prostate cancers do not cause symptoms until they are very large or have spread to other places, often at points when they are incurable. This is why early detection and screening in asymptomatic men is so important. When symptoms do occur they include blood in urine, difficulty urinating, or pain in bones.
Diagnosis
A biopsy is the standard way to definitively diagnose prostate cancer. A biopsy is a procedure in which a small piece of tissue is removed from the prostate and examined under a microscope to check for cancer cells. The doctor may use tests like MRI or a transrectal ultrasound to guide them in selecting where in the prostate the sample should be taken.
Management
Management of prostate cancer depends on the cancer’s stage, how high the risk is, your age, your general health, and your own preferences. The different types of treatment all have their own risks and side effects, so those should be discussed with your doctor and weighed when making a decision about treatment. There are a variety of common treatments for cancer in the prostate as well as some new and experimental treatments.
- Watchful waiting/active surveillance – appropriate for smaller or less aggressive cancers or in men of very advanced age or who have other major health problems
- Surgery – This is the most aggressive form of treatment with highest chances of cure for cancers that have not already spread. This is most commonly done robotically by a surgeon with dedicated training in the technique. The entire prostate is removed, sometimes with lymph nodes for more aggressive cancers. The urinary tract is then reconstructed. With current techniques, hospital stay is usually only 1-2 nights. Surgery is most appropriate for younger men of good health and for more aggressive cancers. Side effects include decline in erections and changes to urinary control which are worst immediately after surgery, then improve with time.
- Radiation – This is also a very good therapy for curing prostate cancer that is still contained to the prostate. Treatment is provided in conjunction with a radiation oncologist who works with the urologist together. Radiation may be delivered by radiation pellets (brachytherapy), external beam, or a combination. Radiation tends to be most appropriate for older men, those with smaller prostates, or those who seek minimal downtime for their treatment. Side effects include decline in erections and changes to urinary control which are usually minimal at first, but progress with time. Sometimes radiation is used in after surgery for the most aggressive cancers or those that recur.
- Hormone Therapy – The goal of hormone therapy with prostate cancer is to lower testosterone. Testosterone is a key growth signal for prostate cancer growth. Hormones are sometimes used in conjunction with radiation to treat cancers that have not already spread. Hormones are more commonly used to slow down and shrink prostate cancers that have spread to other places. Hormone therapy may be managed by the urologist or sometimes by a medical oncologist.
- Chemotherapy – Chemotherapy is not curative but can help shrink cancers and slow their growth. Chemo is most appropriate for cancers that have already spread beyond the prostate. The strongest chemotherapy is given through the veins in conjuction with a medical oncologist who is an expert in the drugs and their potential side effects. Other forms of chemotherapy include oral medications which can be managed by the urologist or a medical oncologist.
Testicular Cancer
Is a cancer that starts in the male gland or testis.
Testicular cancer is most often diagnosed in men ages 15 to 44 years old. When detected early, testicular cancer may be cured.
Risk Factors
Factors that increase testicular cancer risk include a family history of testicular cancer and having undescended testicles or other abnormal testicle growth and development. Other risk factors include race and age. White males are 4 to 5 times more at risk than other races and males between the ages of 15 to 35 are most at risk.
Symptoms
One of the most effective ways to discover a lump is during a testicular self-examination. Discovering a lump or swelling in a testicle is one of the symptoms that young men should be aware of. Others include:
- A heavy, dull or achy feeling in the scrotum or lower belly
- Rarely, individuals may notice soreness or growth in their breasts.
- Signs of early puberty in boys, such as a deeper voice or facial and body hair at a very early age.
In cases where cancer has spread, individuals may experience:
- Lower back or stomach pain
- Difficulty breathing or shortness of breath
Diagnosis
With treatment, the risk of death from testicular cancer is small. Since this type of cancer is seldom painful, men should always see a healthcare provider for an evaluation if they notice a mass or nodule in their testicles.
A urologist will start by evaluating your personal and family medical history followed by a physical examination. The provider may request blood work to screen for certain proteins and hormones made by the cancer.
Treatment
If testicular cancer is diagnosed, imaging will be ordered including a CT scan of the abdomen/pelvis and a chest X-ray. This imaging will help the urologist determine the spread of the disease and the best treatment plan.
Treatment options for testicular cancer include surgery, radiation or chemotherapy. Prompt evaluation is warranted as some forms can be very fast growing